
Is it helpful to talk to an Admiral Nurse? Yes, because Admiral Nurses support family carers and people living with dementia. They are qualified specialist dementia nurses. They are among the MOST valuable resources available to carers (& their family) of somebody with dementia. They support and advise family carers with their knowledge, skills and expertise in dementia care.
This article will provide information on what they do, how they can help you, where to find them, and provide examples of the type of advice/support.
What is an Admiral Nurse?
An Admiral Nurse is a specialist mental health nurse working with families affected by dementia.
Dementia UK provides the Admiral Nurse service. They are a UK charity caring for carers and their loved ones affected by dementia through their specialist Admiral Nurse service.
Admiral Nurses work in partnership with other organisations to extend their reach. For instance, they are referred by GP surgeries, work in hospitals, community/ care homes/hospices and the workplace, e.g. with the NHS, BUPA, etc.
You can also find them as part of the services offered by The Royal British Legion. They provide the Admiral Nurse service to veterans and their families.
How can Admiral Nurses help you as a Dementia Carer?
Admiral Nurses provide one-to-one support and help you with communication problems, dealing with distress, feelings of not coping, and much more.
They give you the tools and skills to deal with the physical, emotional and psychological challenges you might face on your journey caring for someone with dementia. Often, carers refer to them as a lifeline as they passionately help support families.
They can find solutions as dementia progress with their specialist knowledge that those not trained in dementia care may not even consider.
Admiral Nurses provide you with someone to talk to, someone to listen, someone who can advocate for you, someone to who supports you holistically and someone to help you navigate the challenges ahead.
They are a brilliant resource, and unfortunately, not everyone knows about them. You can think of Admiral Nurses as being like Macmillan Cancer nurses. The only problem we have is we need more of them!
So what does that mean?
How Admiral Nurses helped a Carer of a Parent with Alzheimer’s?
I’m a carer of my mum with mid-stage Alzheimer’s, and I’ve been having a tough time with mum’s stress.
Admiral Nurse Kerry Lyons reached out to me after I shared a tweet about my problems. Specifically, I’m having difficulties with mum’s increased anxiety during the day and night. We’ve been in isolation since the Coronavirus hit the UK and in lockdown ever since.
She took the time to emphasise to me that we are living in a challenging time, and I was doing the very BEST for my mother given the current circumstances.
Sometimes you need to hear somebody say that to you to understand you are in a stressful situation. Especially, as we haven’t been apart for months, no respite for me or my mum. Admiral Nurse Lyons told me it’s important to keep reminding myself of this as a carer.
I explained a little more about the types of problems I was facing with my mum’s anxiety during the day and night.
Mum’s anxiety starts before we even reach the bedroom and can escalate to her not sleeping at all. Admiral Nurse Lyons identified that sundowning issues could be a reason for mum being unsettled in her bedroom.
I also believed that mum’s personal care aggravated the situation. It doesn’t help to do all the things necessary for bedtime like hoist her, roll her back and forth, all forceful motions to change her as she’s unable to walk due to a spinal condition. Then say goodnight after all that exertion!
Admiral Nurse Lyons‘ idea was to take a three-fold approach to deal with problems sleeping by creating an emotional anchor, implementing a calming bedtime routine and making sure mum was sufficiently stimulated during the day.
Sleeping Issues
Mum has trouble sleeping in her bedroom because she doesn’t recognise it. Her home was completely renovated to make room for hospital equipment like a bed, fixed hoist, and lift installed.
So her entire room was gutted, repainted and only had room for medical equipment.
Every night mum tells me that this isn’t her room, that she’s sleeping outside, and wants to go home. Her room looks so different now.
I had removed her wardrobes of 40 years that dominated the room. This was huge, with a double wardrobe on each side and an integrated dressing table with drawers. It covered the whole of one side of her room.
After the wardrobe removal, the room felt huge, and when we painted it blue, you could understand why she felt like she was sleeping outside!
Admiral Nurse Lyons nailed the problem when she said, “Her saying the room is too big potentially is … I don’t feel like I belong here”.
I’d focused on making the room medically right and forgotten to ensure she had an emotional connection to the room.
1. Creating an Emotional Anchor
Firstly, Mum needs to get back an emotional connection to the room. Admiral Nurse Lyons suggested adding small touches back into the room, which my mum may not recognise visually but may respond emotionally.
- Adding a soft blanket on the bed to comfort her
- Bringing back her Knick knacks
- Displaying her jewellery and other familiar objects.
- Adding family photographs, pictures she likes onto the wall
- Adding familiar scents
2. Bedtime Routine
Secondly, a bedtime routine can calm and help establish a sleep pattern that could be helpful in the long term. Therefore, she suggested the following steps.
- Reduce stimulations before bedtime by avoiding caffeine-related products, phone/tablet screens, violent or scary programmes before bed
- Just sit and talk with her before starting any personal care, don’t just jump straight into the logistics of getting ready for bed.
- Set the scene, play her favourite gentle music and try singing to her or with her when changing her
- Use your favourite lotions or hand creams and start doing gentle foot and hand massage
- Remove all harsh lighting and use something calmer like a night light with a dimmer switch or use a lamp vs. overhead lighting.
- Use scents like lavender spray in her room or on her pillow to envoke calm environment
3. Daytime Stimulation
Thirdly, Admiral Nurse Lyons focused on the need to keep Mum stimulated and interested throughout the day. I mentioned that mum likes to rip up tissue papers and become distressed, especially in the afternoon, and I find it hard to distract her from it. I get caught up trying to finish day to day activities like cleaning and cooking etc.
I had been very good at keeping mum interested during the day until she suffered from debilitating headaches. So now most activities happen in the morning when we exercise, or mum helps with cooking, or we go out to the garden.
My post, Isolation, also has ideas that I’ve done with mum in lockdown if you’re looking for activity ideas.
And, The Royal British Legion has created this Admiral Nurse activity leaflet with some useful ideas on activities that you could use in lockdown.
Admiral Nurse Lyons also suggested using 3 therapeutic tools to comfort mum when she was distressed or showing signs of it.
1. Doll Therapy
Doll Therapy can help people with dementia by giving them a baby doll or cuddly toy like a teddy bear to cradle and care for.
It’s an effective way for a person with Alzheimer’s or other forms of dementia to reduce stress and agitation.

It’s a controversial form of therapy. Some people don’t like the idea of Doll Therapy and see it as patronising or childlike (that’s my family!), but there are benefits if introduced slowly and in a controlled manner.
For more info, Click to read the Dementia UK leaflet about Doll Therapy.
I still haven’t decided about getting a doll, but I am seriously considering it despite my family’s objections!
2. Twiddle Muff
A twiddle muff is a knitted or crochet muff with bits & bobs attached to it to calm restless hands. It’s stimulation and sensory activity and keeps your hands warm.
Mum & I have been making one for months. Mum is more interested in undoing her knitting, especially if she sees an error. Here’s a pic of how far we got! I’ve given up now on that project!

If you can’t knit, you can buy them on most sites like eBay, Etsy & Amazon, or if an Admiral Nurse has any, they may offer to supply you with one (as in our case!).
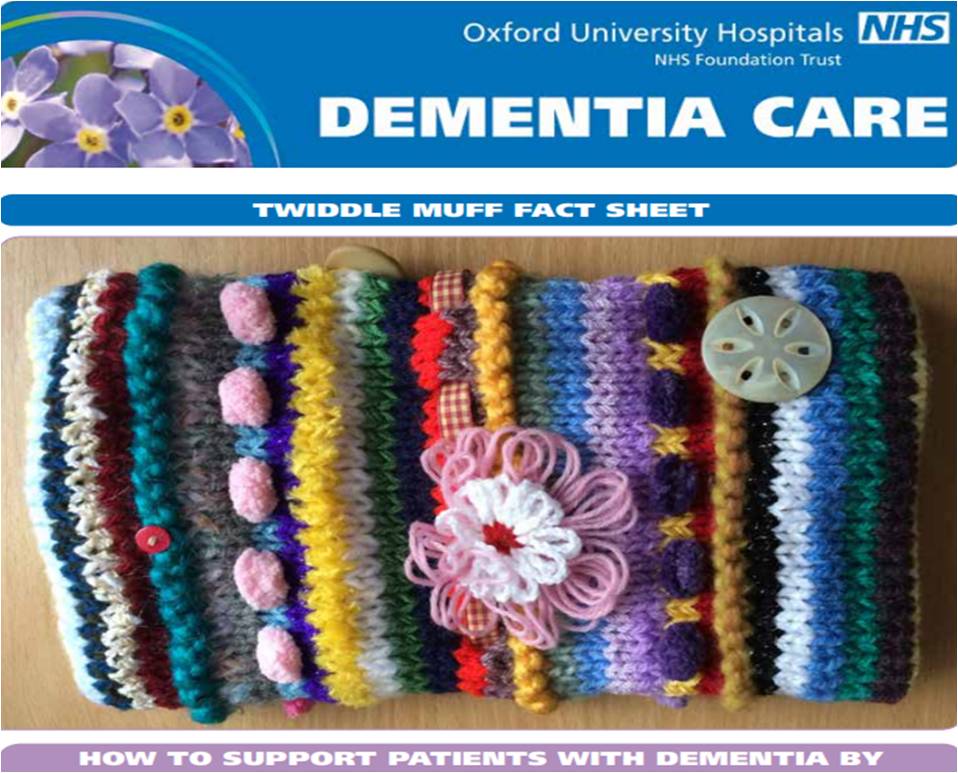
This is the guide from Oxford University Hospitals NHS Foundation Trust of what one should look like, not our failed attempt of making one! Click here to access it.
3. Sensory/ Comfort Blanket
You may not be comfortable with Doll Therapy or a twiddle muff. Maybe then, a sensory blanket similar to a twiddle muff could be a first step for you to try.
They are handy for people like my mum who have busy or fidgety hands. You can make these blankets with textured materials, decorated with objects, zips, or purchased from any sites mentioned above.
We created a fidget blanket from a cushion cover, repurposing materials we had at home rather than creating more waste. You can find the instructions to create your own in my post How to make Dementia Fidget Blanket from a Cushion

How much do Admiral Nurses cost?
Admiral Nurses are FREE! Yes, free! They’re paid for through the fundraising efforts of Dementia UK and donations and support from individuals and other organisations. As such, they are currently limited in number but expanding all the time.
If you want to support their fundraising efforts, then check out their fundraising page. They have some events on most months that you can join to help raise funds for Admiral Nurses! Click here to find out more!
Your support is vital as there are only hundreds of dementia specialist Admiral Nurses compared to thousands of Macmillan Cancer nurses. We need more!
Where can I find an Admiral Nurse?
Dementia UK has a map to help you find your local Admiral Nurse team on their website. Just enter your town or postcode, and they will list the nearest services available to you, including Admiral Nurse clinics that give families specialist advice and support.
You can also get in touch with the Admiral Nurse Dementia Helpline by calling 0800 888 6678. The helpline is open Monday to Friday from 9 am -9 pm and on Saturday and Sunday from 9 am – 5 pm.
You can also contact them by emailing helpline@dementiauk.org.

For more detailed information & other resources available, why not check out the Dementia UK website.
Was it helpful to talk to an Admiral Nurse?
It was extremely helpful to have the help of an experienced professional focusing on the carer’s needs.
Our Admiral Nurse saw things from a fresh perspective. She saw obvious things that I was completely blind to.
Moreover, they also help you to consider new or difficult things to implement, like Doll Therapy.
Admiral Nurses look at your specific situation and provide one to one support, keeping messages simple and refocusing your energy on what’s important for you and the person you care for with dementia.
Having an Admiral Nurse gives you ideas and someone in your corner to turn to.
That’s key. It’s not a one-off consultation. Admiral Nurses are always available for a follow-up to help you.
If you liked this post, let me know in the comments, and why not sign up to subscribe and get notified of new posts by email.














Thanks for sharing your experience and your learning. I had heard about Admiral nurses a while back when researching dementia & trying to prepare for what was to come. I now care for my mum (different kind of dementia to your mum but lockdown & isolation from friends has exacerbated problems for everyone hasn’t it?). I’m there daily for much of the day, but dad is there full-time, 24hrs a day and at 86, with his own health issues, it’s exhausting for him. In different times we’d have been able to call on friends & family to keep each of them stimulated, supported, and having some respite from each other. But unfortunately it’s variously illegal or too risky. I keep thinking my dad needs someone impartial to talk to, and reading your blog has reminded me that there’s an answer. Thank you.
Jo
I’m so glad you found the blog helpful. Yes, this isolation has made life so difficult. At 86, it must very hard for your dad. I’m not sure where you’re located, but give the helpline a call. They can advise over the phone (staffed by Admiral Nurses) or let you know whether any in your area. I’m not sure your situation but can your dad get help through social services by having carers ( can help with meals, meds & personal care). Again they can help advise. Also Age Cymru offer sitting service or can help with someone for your dad to talk to, or chance to get out. Good luck to you, Jo & your parents.