It’s been over a year since Mum had to go into hospital for an emergency. But here we are again!
So Mum was hospitalised on Friday, and it was horrible as always. I can never get used to being taken into hospital. It’s always scary and made much worse now with the COVID.
A lovely ambulance crew arrived. They weren’t rushing us but also had no clue as to why mum was being taken in. They did some basic checks with mum who of course was getting anxious by the sight of the ambulance.
Feeling Unwell
Mum had been feeling unwell since before the new year. We had multiple tests done and antibiotics prescribed but nothing really has been helping. I’d been on and off the phone with the doctor trying to describe mum’s symptoms, & sending in photos.
I had called them out today for a home visit as mum wasn’t responding to me. I couldn’t keep her awake. She lolled being hoisted or even moved, becoming unresponsive to me. It felt like when she was diagnosed with a pulmonary embolism, where we couldn’t wake her at all. So I called our surgery for a home visit because I worried it would get to that stage again.
Before they arrived, I received a phone call from the hospital about the results of our preassessment checks. They told me that they had found something in her blood and that I should call our doctor. Why do that? Why do they scare you instead of just telling you!
“We found something, but can’t tell you, call your doctor”
Luckily our surgery had sent out their home visit paramedic already. As soon as he came in, I told him, and he called the surgery. He informed me that they had found sugars in her blood and that she had diabetes. He took a blood sample, tested it straight away, and said her blood sugars and ketones were too high. The main issue he was concerned about was her ketones. He wanted to hospitalise her as a precaution for a condition called Ketoacidosis.
All I heard was diabetic linked it to obesity in my mind, instantly blamed myself and started crying. Of course, I pulled myself together, buried that deep down to get mum ready.
Hospitalised
We had been hospitalised so many times that I had a bag all ready to go. I just had to replace a few things as they been in there for over a year, add some water bottles and updated the medication list.
The ambulance crew took us to our local hospital, but once there, we had a long wait whilst the medical assessment unit decided whether she should stay or go to the new acute hospital that had opened up. Luckily, we stayed, moved off an ambulance stretcher to a cubicle and then began the long waiting game of being seen by a doctor. Apparently, we had come on the busiest day that they had seen for a while.
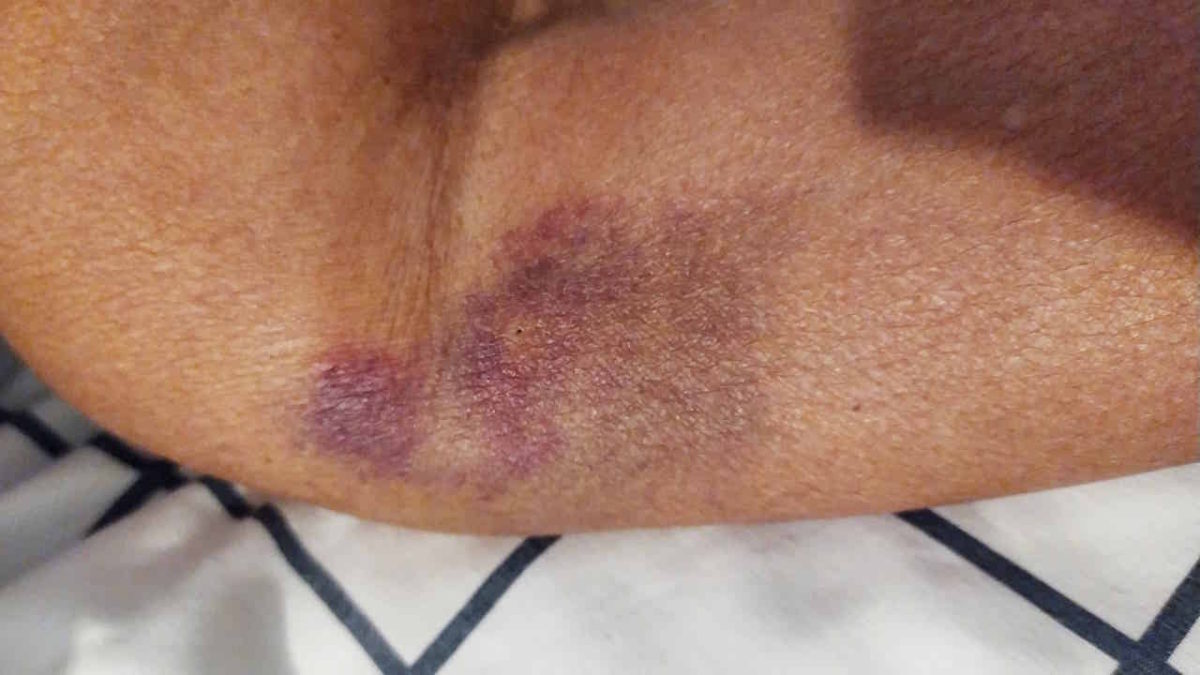
Mum, of course, wouldn’t keep her face shield on (I’d given up on face masks as she spends the whole time pulling it down), and every few hours, they kept taking blood samples and blood pressure tests. Mum hates both. Her blood results kept changing, going up and then down slightly. She fought the nurses constantly trying to take her blood. They gave up on trying to take mum’s blood pressure. It’s always after we get home that we see the bruising from all the blood draws, it never used to happen.
Special Needs Wards
We went in about 3 pm and didn’t speak to a doctor until 1.30 am the following morning.
I kept going to the front desk explaining she had Alzheimer’s, had missed her medications times, not eaten all day but still advised that there were more urgent cases before mum.
I fully understand that but trying to manage mum, who had not been allowed to eat, was getting hysterical in unknown surroundings, had no phone signal so she could be distracted by the family, was tough. I’d brought books, a tablet, knitting, we tried to watch TV, reading a book aloud but nothing worked.
The noises, the beeps, the bangs/clashes as something falls, the cries of other patients all caused mum increasing levels of distress. It was also clear that others with some form of dementia were also here. I was so grateful that they allowed me to stay with her despite the Covid risks.
But I was also critical of the need for a safe space for dementia patients who still hadn’t been looked at in hospitals.
We really need to think about creating spaces as they do with kids for people with dementia. Understandably, that's not now when resources are so stretched, but I hope that they start to think of vulnerable people's needs and have special needs ward in the future.
Diagnosis
When the doctor finally arrived and spoke to us, she was lovely. She explained everything, luckily, diabetes hadn’t affected any major organs, her kidneys were fine, and she didn’t have Diabetic ketoacidosis but she definitely had diabetes. Her ketone level remained high, and they wanted to keep her in to manage to bring them down. We also talked about mum’s possible cancer scare and whether her diabetes could be a risk factor and explain all the bleeding. She didn’t know but would be raising it with our specialist.
Over the last few months, mum has just been unwell, not her usual self. She has suffered from massive headaches, pains in shoulders/legs, multiple UTI’s & thrush causing increased confusion and distress. She’s had unexplained bruising and bleeding. She had swelling in her face, bumps in her mouth and more.
We’d been referred for an exploratory procedure to rule out cancer. For someone without dementia, it could be done awake in a local hospital but for mum, because she is likely to move has to be done under general anaesthetic. Thankfully the preassessment tests taken for that surgery are what identified the sugar in mum’s blood. Who knows how long she had it as she hadn’t been tested for blood sugar in over a year.
Understanding?!
This diagnosis explains a lot the headaches, the thrush, the swelling, lethargy, the pains all linked to increased inflammation because of insulin resistance.
So despite being scared, this diagnosis means that we can start to manage the condition. They started mum on medication at 3 am (the largest pill you’ve ever seen, mum had to break into 3 to swallow it!). They wanted to move mum into a ward, but I refused as they wouldn’t allow me to accompany her. So we stayed where we were until the morning.
I spent the night Googling diabetes and what that really meant. Of course, I had heard about it, but I had no idea how to manage it. In the morning, they retook mum’s blood, and her levels were still high.
Eventually, we saw the consultant (mask under his nose and didn’t take kindly my pointing that out!), and he agreed with the junior doctor’s diagnosis and plans. He accepted my argument for not moving mum to a ward and agreed that we could manage the condition at home and allow us to be discharged.
The only worrying thing was that they provided no advice, no monitoring tools like a blood glucose monitor and were just referred to our doctor. Speak to your GP, and they’ll give you all the information you need. We were told the meds would keep her stable (which clearly wasn’t true as her levels had come down but were still high and variable). Later, I found out that the medications would take a few days/week before stabilising mum’s blood (Google!).
So now we’re home and mum is sleeping, and I haven’t got a clue on what to do, what to feed her, or what the dangers signs are.
What’s next?



Hello Dementia Who, what a scary time, but now you have an explanation for some of the symptoms you had been observing. Hospitals are a challenge, easier to get in than out, well done getting home. I find District nurses are amazing. Though I have not had to deal with diabetes, my dad has wounds on his heels and calf, now an ulcerated tumour behind his ear. He is too frail for treatment, hard for me to accept, but he is generally comfortable.
Thank you Lynn, it always is when going into hospital. One day they will make it easier for those with dementia but until then we can only hope, and highlight the difficulties experienced. I agree our district nurses are great. I’m so sorry for your dad dealing with all those issues, but I’m glad he is comfortable. I worry all the time of mum being in pain, that would be so difficult to deal with again. Thank you for commenting and reading my post much appreciated.